Common Causes of Hip Pain
Osteroarthritis (OA) is sometimes called degenerative arthritis because it is a "wearing out" condition involving the breakdown of cartilage and bones. With osteoarthritis, the cushioning cartilage at the end of the femur may have worn down, making walking painful as bone rubs against bone.
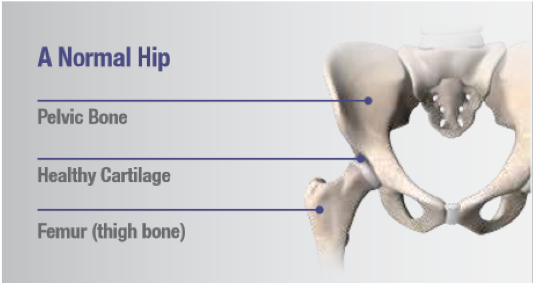
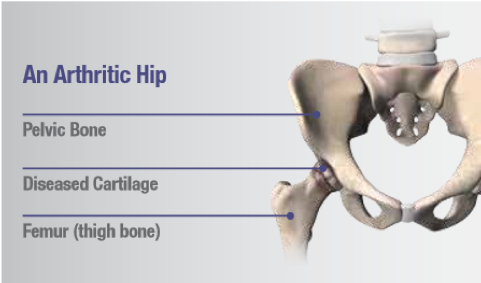
Rheumatoid Arthritis (RA) is an autoimmune disease in which the body's immune response negatively affects the lining of the joints (called the synovial membrane), causing chronic inflammation and pain. The synovium becomes thickened and inflamed. In turn, too much synovial fluid is produced within the joint space, which causes a chronic inflammation that damages the cartilage. This results in cartilage loss, pain, and stiffness.
Avascular Necrosis (AVN) results when bone is deprived of its normal blood supply. Without proper nutrition from the blood, the bone's structure weakens, may collapse and damage the cartilage. Since this is most often seen at the ends of bones, the joints may be greatly affected. This is especially true of the hip joint and most commonly appears at the end of the femur, the long bone that extends from the knee to the hip joint.
RA can affect anyone at any age, but women appear especially at risk. In fact, nearly three times more women are affected than men.1
More than 20,000 people each year enter hospitals for treatment of avascular necrosis of the hip.2
Treatment Options for Hip Pain
The first step towards returning to an active life for people experiencing hip pain could be to schedule an appointment with a surgeon. The orthopaedic surgeon reviews and discusses the diagnosis with the patient. Based on his or her diagnosis, treatment options for hip pain may include:
- Medication
- Joint fluid supplements
- Physical therapy
- Hip replacement
Did you know?
Regular, sensible exercise may help your arthritis. Arthritic joints sometimes need a short period of rest followed by a gradual return to activity. It’s important to maintain your strength and range of motion in your joints.3
IMPORTANT INFORMATION
Disclaimer
Hip joint replacement is intended for use in individuals with joint disease resulting from degenerative and rheumatoid arthritis, avascular necrosis, fracture of the neck of the femur or functional deformity of the hip.
Knee joint replacement is intended for use in individuals with joint disease resulting from degenerative, rheumatoid and post-traumatic arthritis, and for moderate deformity of the knee. Joint replacement surgery is not appropriate for patients with certain types of infections, any mental or neuromuscular disorder which would create an unacceptable risk of prosthesis instability, prosthesis fixation failure or complications in postoperative care, compromised bone stock, skeletal immaturity, severe instability of the joint, or excessive body weight.
Like any surgery, joint replacement surgery has serious risks which include, but are not limited to, pain, bone fracture, change in the treated leg length (hip), joint stiffness, hip joint fusion, amputation, peripheral neuropathies (nerve damage), circulatory compromise (including deep vein thrombosis (blood clots in the legs)), genitourinary disorders (including kidney failure), gastrointestinal disorders (including paralytic ileus (loss of intestinal digestive movement)), vascular disorders (including thrombus (blood clots), blood loss, or changes in blood pressure or heart rhythm), bronchopulmonary disorders (including emboli, stroke or pneumonia), heart attack, and death.
Implant related risks which may lead to a revision of the implant include dislocation, loosening, fracture, nerve damage, heterotopic bone formation (abnormal bone growth in tissue), wear of the implant, metal sensitivity, soft tissue imbalance, osteolysis (localized progressive bone loss), audible sounds during motion, and reaction to particle debris.
The information presented is for educational purposes only. Speak to your doctor to which therapy is appropriate for you. Individual results vary and not all patients will return to the same activity level. The lifetime of any joint replacement is limited and depends on several factors like patient weight and activity level. Your doctor will counsel you about strategies to potentially prolong the lifetime of the device, including avoiding high-impact activities, such as running, as well as maintaining a healthy weight. It is important to closely follow your physician’s instructions regarding post-surgery activity, treatment and follow-up care.
Speak to your doctor to decide which therapy/treatment is appropriate for you.
Stryker Corporation or its other divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: Mako, Stryker, Together with our customers, we are driven to make healthcare better. All other trademarks are trademarks of their respective owners or holders.
GSNPS-PE-85_17642
REFERENCES
1. Arthritis Foundation website, http://www.arthritistoday.org/aboutarthritis/types-of-arthritis/rheumatoid-arthritis/what-you-need-toknow/what-is-ra.php, accessed September 2014
2. AAOS website, http://orthoinfo.aaos.org/topic.cfm?topic=a00216, accessed July 2015.
3. Cleveland Clinic website, http://health.clevelandclinic.org/2012/08/six-myths-about-joint-painand-arthritis/, accessed October 2014